Cartilage injuries in the knee or shoulder can significantly impact mobility, function, and comfort. Unlike many other tissues, cartilage has a limited ability to heal on its own, so damage can become long-lasting. If untreated, cartilage injuries may lead to pain, reduced activity, and even early-onset arthritis. Fortunately, modern cartilage restoration procedures can repair or replace damaged tissue, preserve joint function, and help patients maintain an active lifestyle. This guide explains how these procedures work, who may benefit, and what to expect during recovery.
Quick Answer: How Do Cartilage Restoration Procedures Protect Joint Function?
Cartilage restoration procedures repair or replace damaged joint cartilage to relieve pain and protect long-term joint function.
Treatment options may include:
- Microfracture surgery
- Osteochondral autograft transfer (OATS)
- Autologous chondrocyte implantation (ACI)
- Osteochondral allograft transplantation
- Arthroscopic cartilage repair procedures
In some cases, non-surgical treatments such as physical therapy may also support healing and reduce symptoms.
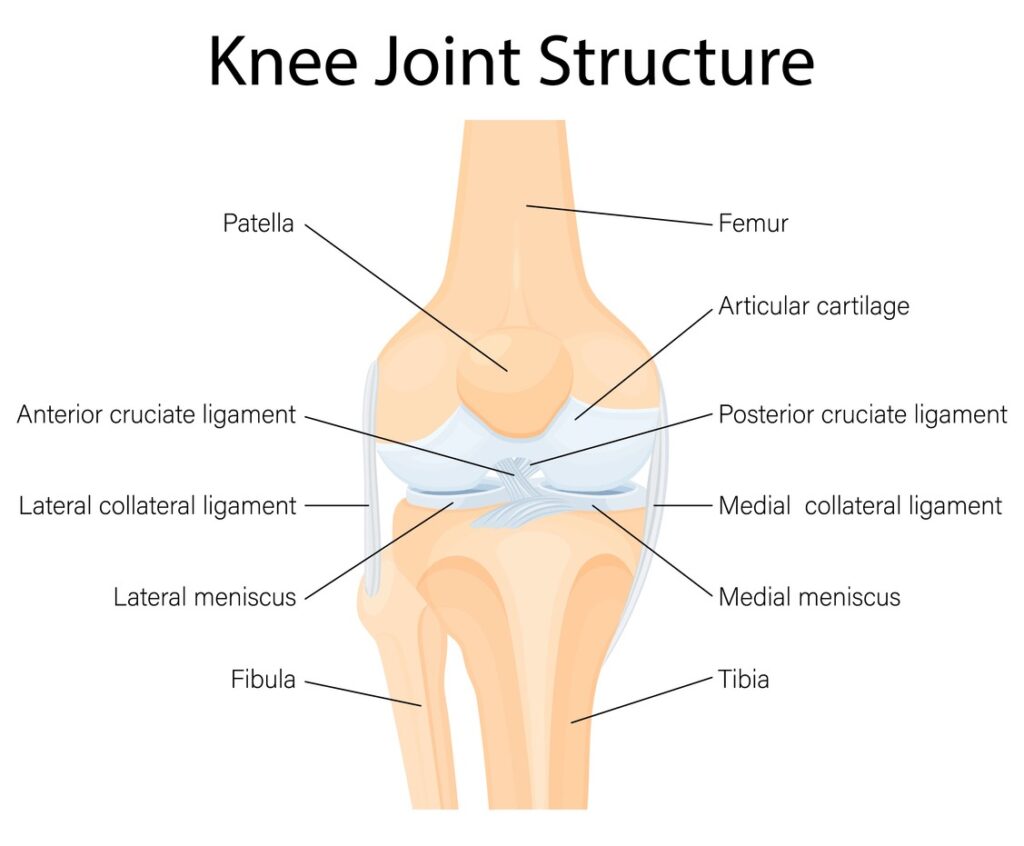
What Causes Cartilage Damage in the Knee or Shoulder?
Cartilage can be damaged by trauma, overuse, or degenerative changes. Common causes include:
- Sports Injuries: Sudden twists, falls, or direct impacts can shear or tear cartilage in the knee or shoulder, often causing pain, swelling, and reduced joint function.
- Repetitive Joint Stress: Activities like running, throwing, or lifting repeatedly stress the joint, gradually wearing down cartilage.
- Age-Related Degeneration: As we age, cartilage naturally thins and loses its elasticity, making it less able to absorb stress and more susceptible to injury.
- Previous Surgery or Trauma: Areas that have experienced prior injury or surgical procedures may have weakened or scarred cartilage, which can lead to further deterioration.
- Inflammatory or Joint Conditions: Chronic inflammation, such as arthritis can erode cartilage, causing pain, stiffness, and decreased joint mobility.
What Are the Symptoms of Cartilage Damage?
Cartilage damage in the knee or shoulder can produce several noticeable symptoms. Recognizing these signs early can help prevent further joint deterioration.
- Pain During Movement: Persistent discomfort or aching in the joint during activity or exercise may indicate that the cartilage is worn or irritated.
- Swelling or Stiffness: Joints may feel swollen, tight, or difficult to move after activity, signaling inflammation or underlying cartilage damage.
- Catching or Locking: A sensation of the joint catching, clicking, or locking during motion can suggest loose cartilage fragments or uneven joint surfaces.
- Instability or Weakness: Feeling that the joint may “give out” or is unstable can occur when damaged cartilage affects joint support and function.
- Reduced Range of Motion: Difficulty fully bending, straightening, or rotating the joint may be an early warning that cartilage is compromised.
Who Is at Higher Risk for Cartilage Injuries?
Several factors increase the likelihood of developing cartilage damage.
- Athletes and highly active individuals may experience repetitive stress on joints from running, jumping, or throwing.
- Sudden traumatic injuries can also tear cartilage and cause knee instability.
- Age-related cartilage degeneration is another common factor. As cartilage loses elasticity over time, it becomes more susceptible to wear and injury.
- Previous joint injuries, surgeries, or chronic inflammatory conditions like arthritis can also increase the risk of cartilage deterioration.
Understanding these risk factors allows patients to take proactive steps to protect their joints and maintain long-term mobility.
What Are the Treatment Options for Cartilage Damage?
Protecting joint health involves a combination of lifestyle habits, non-surgical treatments, and, when necessary, cartilage restoration procedures.
- Physical Therapy: Targeted physical therapy and strengthening exercises around the joint help reduce stress on cartilage, improve stability, and support long-term joint function.
- Low-Impact Exercise: Swimming, cycling, and resistance training preserve mobility without stressing the joints and strengthen surrounding muscles.
- Weight Management: Maintaining a healthy weight reduces pressure on cartilage and helps slow joint damage.
- Medications: Anti-inflammatory medications may reduce pain and swelling temporarily.
- Shockwave Therapy: This non-surgical treatment uses focused sound waves to stimulate healing in surrounding soft tissues, reduce pain, and improve joint function.

What are the Types of Cartilage Restoration Surgery?
When cartilage damage is severe or symptoms persist despite conservative care, surgical intervention may be necessary. Procedures include:
- Microfracture: Small holes are created in the bone beneath the damaged cartilage to stimulate the growth of new cartilage-like tissue, helping restore the joint surface and reduce pain.
- Osteochondral Autograft Transfer (OATS): Healthy cartilage and underlying bone are taken from one area of the joint and transplanted to the damaged site, promoting repair with natural tissue.
- Autologous Chondrocyte Implantation (ACI): Your own cartilage cells are harvested, grown in a lab, and implanted into the damaged area, encouraging the development of durable, functional cartilage.
- Minimally-Invasive Arthroscopy: Small incisions allow surgeons to precisely remove or repair damaged cartilage, smoothing the joint surface while minimizing tissue trauma and shortening recovery time.
- Osteochondral Allograft Transplantation: Donor cartilage and bone from a tissue bank are used to replace larger areas of damaged cartilage, restoring joint function in cases where autografts are insufficient.
What are the Healing Challenges for Knee and Shoulder Cartilage?
Cartilage in the knee and shoulder is particularly vulnerable because these joints experience high loads and frequent movement. In the knee, cartilage helps absorb impact from walking, running, jumping, and twisting motions, protecting the bones and ensuring smooth joint motion. In the shoulder, cartilage cushions the glenohumeral joint and facilitates a wide range of overhead movements, including throwing and lifting. Unlike other tissues, cartilage has a limited blood supply, which slows natural repair and makes it more difficult for injuries to heal on their own. This makes early treatment important for preserving joint function.
When Should You See a Doctor for Cartilage Damage?
Consulting a healthcare provider promptly can help prevent further joint deterioration and preserve function. You should see a specialist if you notice persistent joint pain that interferes with daily activities, swelling or stiffness that doesn’t improve, locking or catching sensations, or weakness and instability in the knee or shoulder. Early evaluation allows your provider to recommend a personalized plan, which may include non-surgical therapies like shockwave treatment, targeted rehabilitation, or surgical intervention to restore function and reduce the risk of long-term complications.
Cartilage Restoration Treatment at Peter Howard, M.D.
If you are dealing with knee or shoulder pain from cartilage damage or suspect you may benefit from cartilage restoration, our team at Peter Howard, M.D. is here to help. We provide thorough evaluations and develop personalized care plans tailored to your specific needs, whether that involves conservative therapies, shockwave treatment, or surgical procedures. Our goal is to relieve pain, restore joint function, and help protect long-term mobility so you can safely return to daily activities, sports, and exercise. Reach out today to schedule an appointment and take the first step toward healthier, stronger knees and shoulders so you can move freely and with peace of mind.


